News & Publications
Putting patients first: How Saskatchewan’s COVID-19 vaccine delivery was made faster, better, and more patient-centered
Feb 10, 2022
Categories: News
Saskatchewan residents may have noticed many improvements in clinic design and vaccine delivery when receiving a dose of the COVID-19 vaccine in 2021.
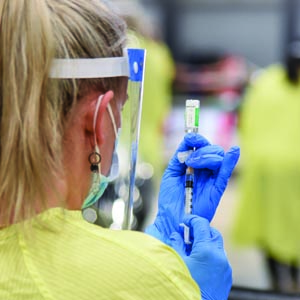
That’s because a team of continuous improvement specialists and health-care employees from across the Saskatchewan health system were working night and day, both behind the scenes and in the clinics themselves, as part of the early mass vaccination plan.
One of the many improvements the task team introduced was a “patient-first” approach to vaccine clinic design. This model aims to build the health-care experience for the patient and to ensure that health-care providers can reliably carry out the most important patient-care tasks with ease.
Here are some of the results from four immunization sites:
- The care came to the patient instead of the client moving to each step, which was more convenient and safer for the patient;
- Immunizers noticed their work was now more efficient; and
- There was reduced need for space, staff, and supplies so resources were saved, along with countless lives.
The task at hand
In early 2021, the 28-member task team began working daily on two objectives:
- First, to ensure that 206 vaccine clinics across the province were ready by March 15, 2021; and
- Second, to safely and efficiently ramp up services as vaccine supply increased.
The forecasted demand was 900,000 people who would be eligible for immunization, and would need two doses each over 180 days. That worked out to 10,000 doses per day every single day.
On the supply side, the health system would need a large pool of employees to deliver those vaccines into arms, and those same employees were also needed elsewhere across the system as cases and hospitalizations rose. To ensure success, the improvement task team knew they had to help immunizers and clinic managers develop reliable and easy processes to safely meet vaccine demand.
The sooner vaccines were administered during this pandemic, the more lives that would be saved. As 3sHealth’s Senior Physician Consultant and task team member Dr. Joy Dobson puts it, “a COVID vaccine in your arm can save your life, and a COVID vaccine in everyone’s arm can save our way of life.”
One of the most innovative changes was to redesign the care delivery model to improve both safety and efficiency.
From traditional to patient-first vaccine clinic design
Patients left with the right vaccine in their arm and a better experience. Providers were able to apply the model to any clinic size and the work was made reliable and easier. Costs came down as we needed fewer supplies, less space, and fewer skilled employees desperately needed elsewhere.
Kristin Mitchell describes patient-first design as a “paradigm shift.” Mitchell is a Saskatchewan Health Authority’s Planning and Performance Measurement Specialist and she was the task team’s lead quality improvement specialist for the Regina area.
“The implementation of the Saskatchewan patient-first clinic design addressed the three voices of continuous improvement – the voice of the patient, of the process for health-care providers, and of the business,” explains Mitchell. “Patients left with the right vaccine in their arm and a better experience. Providers were able to apply the model to any clinic size and the work was made reliable and easier. Costs came down as we needed fewer supplies, less space, and fewer skilled employees desperately needed elsewhere.”
In the traditional clinic design, the patient would first register and then move to the vaccination area. After receiving their vaccination, the patient would get up and walk over to the observation area for a 15 minute safety wait to ensure there were no adverse effects from the immunization. This design required a lot of movement on the patient’s part. It also reduced visibility between the registration, vaccination, and observation areas.
The task team was able to create a patient-first design where, after registration, the patient would move to a single chair. Then, the immunizer would come to the patient and administer the vaccine. The patient would stay in the same chair for their observation period.
“The majority of vaccine reactions happen early on, exactly when we are asking clients to get up and move,” notes Dr. Dobson. “The patient-first design allows the client to stay where they are for their observation rather than walking to another spot, avoiding the risk of fainting while upright.”
“It was also easier for all health-care employees at the clinic to observe everyone, and so we could spot anyone in trouble, whether that was a patient who needed some assistance, or an employee who was requesting supplies or help.”
Patients surveyed about their experience with the redesigned clinic had the following to say:
- “I am much happier to just stay in my seat. To not have to get up and down one extra time is much better for my knees. I also feel more comfortable being in the room with the nurses. I was very nervous last time.”
- “This is far more convenient. It is so clean and efficient.”
- A daughter of a second dose recipient said she had seen a report on the news of a vaccine delivery model in Canada putting patients at the centre and making the process more efficient. “I thought, why aren’t we doing this?” she said. “Then, I was surprised when we arrived today and I was so happy. To be able to free up nurses is wonderful. The whole process was great. It was good before too but good on Saskatchewan for doing something to make things better.”
Immunizers also benefited from the new process. They were able to adjust their work based on their increased visibility of clients. The new process also assigned some of the sanitation tasks to support staff, freeing up the immunizers to administer vaccines more efficiently. Before the improvement, it took between seven to 10 minutes to administer each dose of the vaccine. Improvements reduced that time to four to five minutes for each vaccination.
“The task team was intensely focused on getting to where the work was done and hearing from the health-care employees staffing the clinics,” says Mitchell. “In fact, most improvement ideas we implemented came from front-line employees and clients during over 60 improvement sessions we ran.”
“I would like to thank the quality improvement team and all of the front-line employees we worked with for their collaboration, contributions, and for their ongoing commitment to quality, safety, and continuous improvement for all Saskatchewan patients.”
79,657 lives positively impacted
In 2016-17, 3sHealth developed a methodology to track the quality effects that shared services have on patients. 3sHealth has a target of positively impacting 1.2 million lives by 2025. To date, health-system partner organizations have positively impacted the lives of 1,030,009 citizens in Saskatchewan.
This patient-first clinic design improvement work positively impacted 79,657 lives in Saskatchewan according to 3sHealth’s methodology.
In order for an improvement to positively impact a life, it needs to make a demonstrated improvement to quality of care in terms of safety, timeliness, effectiveness, efficiency, equity or reliability, or patient-centredness; the Institute of Medicine defines these as the six dimensions of quality. 3sHealth then calculates the number of lives health system initiatives positively impacted with health system data after input from internal audit expertise.
Here is the simple summary of how 3sHealth calculated 79,657 lives positively impacted by this improvement work:
- As of Dec. 9, 2021, the patient-first clinic model was in use in four clinics in Saskatchewan, including the mass clinics in Regina and Saskatoon. From the first patient-first clinic launch in spring until the data pull date, 159,314 doses were given at these clinics. The lives impacted number assumes that all of these patients attended the same clinic twice over the measurement period to become fully vaccinated, therefore counting the overall improvement as one life impacted per two doses. Halving the number of doses to calculate the lives impacted number ensures it is a conservative figure as some people may have received doses at other clinics.
The Saskatchewan spirit of innovation
The task team learned a lot from the “Hockey Hub” model developed in Ontario’s Grey Bruce Public Health unit. In turn, people in Saskatchewan and around the world were able to benefit from the work the provincial task team had done. As Mitchell explains, “We were sharing our continuous improvement ideas and learnings with vaccine clinics elsewhere in the world through weekly webinars.”
This patient-first clinic redesign is one of many efforts fighting COVID-19 that exemplified the Saskatchewan spirit of innovation. Here are some other examples:
- Success of Saskatchewan’s drive-thru vaccination clinics shared;
- Impressive SHA scheduling tools contributed to vaccine clinic success, will be featured in AIMS;
- Inside one of Saskatoon’s drive-thru COVID-19 testing centres;
- Saskatoon field hospital now COVID-19 mass immunization site; and
- Tools from forthcoming provincial information management system provide valuable insight for COVID-19 response.
Haven’t received your vaccination yet? Don’t hesitate, vaccinate! Book here today.